Intradialytic Hypotension: Why Blood Pressure Drops During Dialysis Sessions
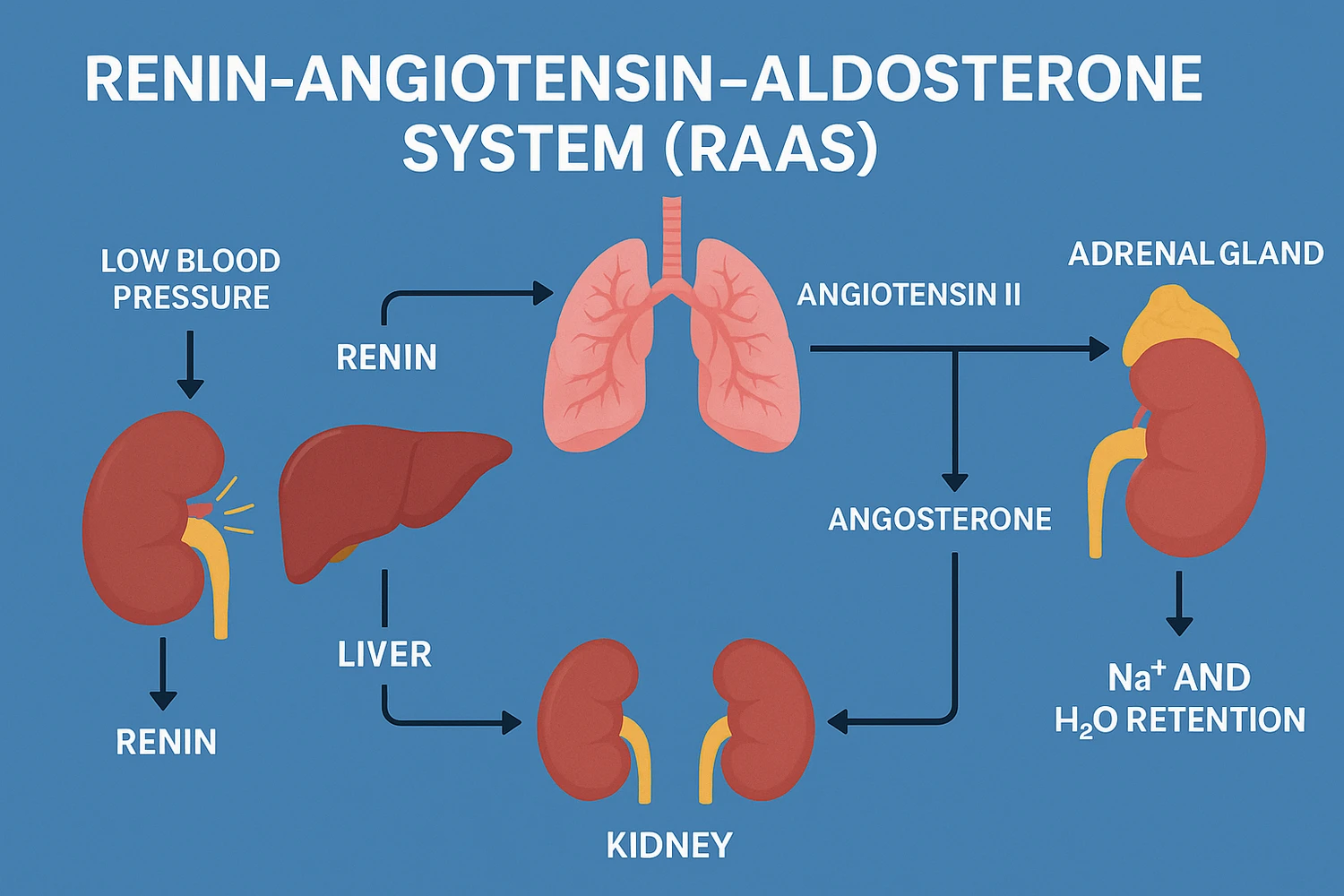
Intradialytic hypotension occurs because dialysis imposes a controlled but aggressive physiological stress on the cardiovascular system, primarily through the removal of intravascular fluid. As ultrafiltration progresses, circulating blood volume decreases, which reduces venous return to the heart and subsequently lowers cardiac output. Under normal conditions, this would be compensated by sympathetic activation, vasoconstriction, and hormonal mechanisms such as the renin–angiotensin–aldosterone system, but in many dialysis patients these compensatory responses are impaired due to autonomic dysfunction, diabetes, cardiovascular disease, and the effects of medications.
At the same time, dialysis induces changes in plasma osmolality and vascular tone, causing fluid to shift out of the vascular compartment into surrounding tissues, further exacerbating the reduction in effective circulating volume. The combination of reduced preload, limited cardiac reserve, and impaired vascular response creates a tipping point where the body can no longer maintain blood pressure, resulting in a sudden drop during the session.
Nexev is designed to intervene before this tipping point is reached by reframing the problem as one of real-time physiological trajectory rather than static measurement. Instead of relying on intermittent blood pressure readings and reacting after a drop has already occurred, the system continuously integrates machine parameters such as ultrafiltration rate, blood flow, arterial and venous pressures, and dialysate composition with patient-specific factors including baseline haemodynamics, comorbidities, and prior session responses.
By modelling how these variables evolve over time, Nexev identifies patterns that indicate a declining compensatory reserve, effectively detecting when the patient is approaching haemodynamic instability before it becomes clinically apparent. This enables earlier and more precise adjustments to dialysis parameters, allowing fluid removal and treatment conditions to be modulated in a way that maintains circulatory stability, reduces the likelihood of abrupt blood pressure drops, and transforms dialysis from a reactive protocol-driven process into a proactive, patient-specific system.
Back to top